Q: What causes the skin changes in psoriasis?
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
A: The outer layer of the skin, known as the epidermis, contains skin cells which regenerates continuously. The process normally takes three to four weeks, but in psoriasis, the skin cells divide more quickly so that the cells both form and shed in as little as three to four days. This gives rise to psoriasis plaques which are well defined and slightly raised pink or red areas with silvery white scales.
Several patterns of psoriasis exist. The most common type is chronic plaque psoriasis, where you get the large plaques usually present on the knees, elbows, trunk and scalp.
Then there's guttate psoriasis, which consists of small plaques of psoriasis scattered over the trunk and legs. It can be caused by a bacteria called Streptococcus, which causes throat infections.
There is also palmoplantar psoriasis, affecting the palms and soles.
Another subtype is pustular psoriasis, which is a rare type of psoriasis where plaques are filled with tiny yellow spots. It can be localised or generalised and can flare rapidly, resulting in hospital admission.
Erythrodermic psoriasis is a rare aggressive form of psoriasis affecting nearly all of the skin and can require hospital admission for treatment.
About half of psoriasis patients have psoriatic nail disease with nail pitting as the most common change.
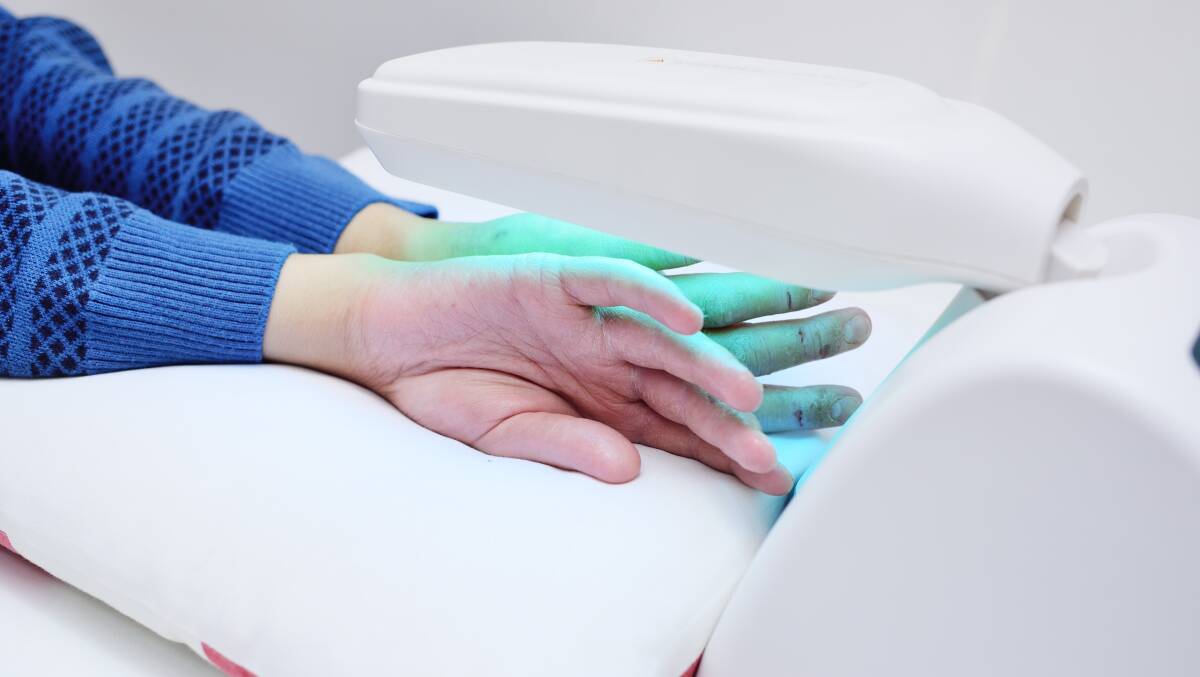
Treatment varies according to condition severity and individual circumstances. Topical treatment is sufficient in most patients. For people with more extensive or difficult to treat psoriasis, phototherapy, tablet treatment or injectable treatment may be considered.
Topical treatment consists of creams, ointments, gels and lotions. Phototherapy is ultra violet light delivered in a controlled way. Tablet treatment include oral agents that either suppress the immune system or a vitamin A related tablet to slow down proliferation of skin cells. Injectable treatment consists of biologics treatment which are medications made from human or animal proteins. They are designed to specifically target biologic pathways that cause inflammation in the skin and other organs.
What is psoriasis?
Psoriasis is a common and stigmatising chronic inflammatory skin disease. It affects about 2 per cent of the population worldwide, and it is certainly more than skin deep: psoriasis may coexist with psoriatic arthritis and may also be associated with a number of other comorbidities including Crohn's disease, diabetes mellitus, obesity, cardiovascular disease, depression and metabolic syndrome. Hence it is a major public health problem and has a negative impact on an individual's quality of life.
Psoriasis is a complex condition resulting from the interplay of genetics, environmental and immunological factors. Twin and family studies have shown that psoriasis has a strong genetic component although the inheritance pattern is unclear. Genetic studies support the notion that multiple gene products share a role in the immune regulation of psoriasis, contributing to disease pathogenesis.
People with psoriasis may withdraw from public life because of embarrassment of how they look, but also from losing the ability to work or exercise. This can mean they are also unable to look after their own condition. Holistic management of psoriasis is important to help improve the affected individual's quality of life.
For more information on psoriasis visit the Australasian College of Dermatologists website.
- Answer provided by Melbourne dermatologist Dr Rose Mak, through HealthShare, a digital company dedicated to improving the health of regional Australians. Submit questions, and find more answers, at healthshare.com.au.

